Spring has sprung in Seattle and it’s just beautiful. Brad and I got lucky and missed the worst of winter while we were on the road filming the documentary. We left before sunrise Jan 12 and got home end of day Feb 14. Definitely slower than flying but safer. We stayed in self-check in AirBnBs with only occasional masked trips to the supermarket – no more exposure than at home.
The interviews we collected were beyond our expectations and well worth any discomfort! It was such a metabolic fangirl dream!
- Seeing my hero, Travis Christofferson, twice in one year (he’s, like, my best friend now)
- Spending time in Seyfriend’s lab (!!!!)
- Meeting Dr. Robert Weinberg in person!
- Being blown away by Dr. Angela Poff, Jess Kelley, and Dr. Charles Meakin in the flesh – and surprise star Sam Apple.
I won’t spent too much time on it here but you can see some early footage samples on the documentary site.
We’d initially delayed the trip so that I could have my scans first. Unfortunately, American healthcare subverted my plan. (My scans were on Jan 4, the first business day of the new year, I had new insurance that hadn’t authorized in time so I needed to pay the discounted rate of $8,500 first and then work with insurance to reimburse… Haha, yeah right. For the record, those same scans cost me $0 in Hong Kong where I’m a resident, $1,500US out of pocket at a private hospital in Europe where I’m a medical tourist, and $0 in Europe at a hospital where I’m a tourist with an emergency. American healthcare is a tragic joke.)
But whatever, I rescheduled my scans for after the trip.
My seizures had been increasing and I knew it would be a stressful trip so I started taking steroids (dexamethasone) and anticonvulsants (Keppra). The seizures improved but the side effects, especially the first 3 weeks of Keppra, were almost unbearable. I’ve adjusted now and, except for the typical steroid moonface, side effects are minimal. However, I’ve had increasing breakthrough seizures.
The results
Based on seizure activity, I knew my scans wouldn’t be great so I wasn’t shocked to learn that my cancer is back – first signs since October 2019 (although I haven’t had an MRI since September 2020 and, with 20/20 hindsight, you can kind of see one forming).
- Of the two areas of radiation necrosis in my brain, once appears smaller and the other slightly larger (although the swelling around it is reduced).
- I have two new areas of cancer progression in the brain. Docs think it looks like leptomeningeal disease (which would be bad) but that’s what they said last year about my radiation necrosis.
- My body is still cancer-free.
So, what now?
Not much for now.
Destress
The trip – heck, the move to the US – was stressful so I’m keen to get back to my healing lifestyle. Brad went alone to LA for some work so I could stay here in retreat and get back to yoga, meditation, and HBOT which I’d been missing.
On which note, I’m overwhelmed to have so many kind supporters. I apologize that I may not be able to send a reply to everyone who reaches out but I’m grateful for your support.
Fast
I kicked off an extended fast. My last extended fast was 9 days in June 2020. Brad and I have kept our routine of water fasting every Monday and the first Monday-Wednesday of each month. This time I’m aiming for at least two back-to-back 7 day fasts with a refeed in between (2×7 is safer than 14 days straight). I’m halfway through (refeed was yesterday) already feeling hugely improved in the side effect department.
HBOT
I first really came to understand radiation necrosis in February 2020 when Dr. Seyfried gave a presentation at the Metabolic Health Summit explaining how it causes progression of brain tumors. He was passionate when when explained that radiation is one of the quickest ways to speed death from brain tumors.
This was right after I’d been diagnosed with a new lesion in my brain and was hopeful it was radiation necrosis from my two previous radiosurgeries, and not a new tumor. I know it wasn’t Tom’s intention to scare anyone but he made it sounds swift and inevitable. One of my oncologists, Chuck Meakin, was behind me in the audience and patted my shoulder after the presentation saying, “that won’t be you.”
Seyfried’s research has nevertheless left no doubt that my radiation necrosis is feeding my cancer. I had 55 HBOT dives (90 minutes at 2.0atm) before we left on our trip in an attempt to treat it. I’d gotten a little zesty and given myself oxygen poisoning and I actually needed the month off for my lungs to heal – the trip was perfect timing. I’m happy to be back at it, diving a little more modestly. While I’d hoped my scans would show better results in the radiation necrosis department, at least the small improvement was encouraging and taking steroids concurrently has been shown to make it a more effective treatment.
Up the TKI
I had been taking a half dose, the minimum effective dose, of lorlatinib for almost a year. The doctors never told me and I foolishly didn’t bother looking it up until last week, but dexamethasone, which I starting taking for seizures 2 months ago, reduces the effectiveness of lorlatinib. So yeah, I’ve been taking less than the effective dose of my cancer medicine for 2 months.
I admit that I’m a little pissed about this one since my docs know I was on a reduced dose until I can line up funding ($20,400 a month here in the US, $20 a month in Honk Kong) and that my current supply is expired.
So I’m now taking a full dose (still expired) and hoping that the steroids don’t block too much. Fasting has also been shown to improve efficacy – it certainly reduces the side effects! If I haven’t developed resistance to lorlatinib, this correction could be what I need.
But then what?
Targeted therapy resistance was a common theme in our documentary interviews. Everyone knows that these absurdly expensive therapies work for a handful of people and for a short time.
My first TKI, crizotinib, saved my life in those early days that were very touch and go. It bought me 4 months to get my footing and learn about the metabolic therapies that could make these treatments more effective. It has an average duration of 14 months before resistance kicks in but, again, it was only 4 for me. It didn’t matter, anyway, because it doesn’t work in the brain.
When I started taking lorlatinib 23 months ago, it had an average duration of 8 months before resistance. By then I knew about fasting, keto, stress reduction… not only did it buy me time, it bought me “no evidence of disease” and almost two years progression free. More than I ever had right to expect.
I personally think I have more time with lorlatinib but I’ve never stopped having a backup plan. It’s just evolved with the circumstances.
- More radiation is out. That’s the standard treatment but, given my past tendency for radiation necrosis, even my doctors aren’t pushing me too hard. I know more radiation would just spread more cancer while being overall unpleasant.
- Immunotherapy is out. Although I have a high PD-L1 expression, it’s generally not effective for people with my mutation so insurance would never pay and I could never afford it.
- Other TKIs are out. There are a few trials that I’m not currently eligible for but nothing else out there that treats the brain.
My next step would be conventional infusion chemotherapy. I think I would rock it. But generally I don’t intend to attempt any desperate treatments for a few extra weeks of life and a whole lot of debt for Brad.
The end game
This has never been curable.
I never expected to see the end to Game of Thrones (and sometimes wish I hadn’t). And yet, I have spent the past 2 and a half years healthier than I’ve ever been, travelling the world, developing as a person and just loving life. I can’t get over how lucky I am.
I believe I have much more time left but death is inevitable. For everyone. I’m not afraid of it, I just have a whole lot to get done first.

I don’t have a date for my next scans yet but probably early May. I’m hitting the road for our next three documentary interviews at the end of March through early April. Then I just have to figure out how to get into Canada.
I’m no longer taking on clients but I’m working on a series of online classes and a book presenting a more organized version of what I’ve learned about implementing the up-to-date research from experts in the field. Like I said, a whole lot to get done.
April Update
Evidently I met with my doctor before he had the full results of my scans. I also think he may have forgotten my Hong Kong history (understandable). All four lesions in my correspond with one of my four previous treatment areas:
- Left parieto-temporal (treated with SRS 11/2018)
- Right cerebellar (treated with SRS 11/2018)
- Right temporal (treated with SRS 4/2019)
- Left temporal (treated with SRS 4/2019)
On a hunch, I went to a lab to test my tumor markers and they’re both deeply normal. Now, this isn’t definitive which is why my doctors won’t test them, but it really makes me think I’m still dealing with expanding radiation necrosis and not cancer recurrence. Docs think it looks like leptomeningeal disease but that’s exactly what they said in Dec 2019 for the first lesion that I proved was necrosis.
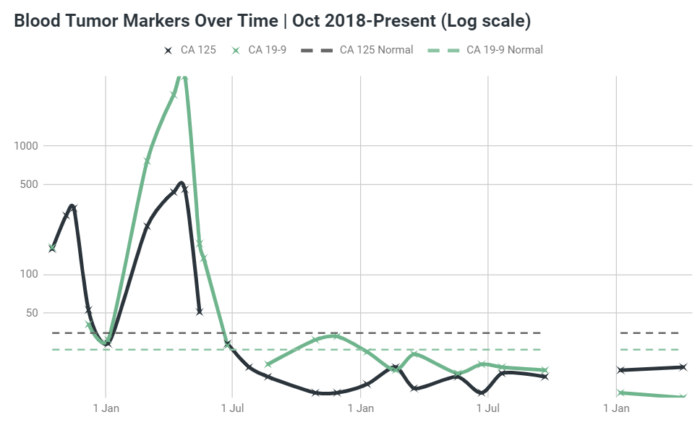
I just had fresh scans yesterday and requested a consult later to make sure my docs have seen the results. I’ll update you when we know more…







16 comments
Maggie – I’m sorry to hear this news. Your knowledge of the entire subject is mind boggling to me. The determination you have and the ability to stay so positive is inspirational. My prayers to your continued healing. ♥️
Thank you, Deb! Honestly, I feel as good today as I ever have and am savoring the present moment. I wouldn’t trade this experience for anything
The cost differences between countries is absurd. I hope that gets driven home in the documentary.
I wish! Sadly not a topic for this doc but next one! It really is absurd.
You are a machine! I love your approach! You are so ON! Thank you for being so determined and modeling such an amazing attitude towards all your challenges! Thank you for sharing your plan of action! We are in this together! What an amazing trip! What an amazing life you live! So vibrant! So passionate!
Nate, thank you for being my biggest cheerleader through all this! I can’t imagine what it’s like from your perspective. I feel right there next to you three, reveling in this amazing life!
Thank you for this update, Maggie! Thinking about you daily. So devastated to hear about the new areas of progession in the brain. And as always, so amazed over your ability to get action oriented and having a positive mindset. Truly thankfull for all the work you have done and are doing with the blog, Instagram, the documentary, and now also a book!!! However, so glad that you will take some extra time to destress and focus on your healing. Sending loads of love and healing thoughts your way.
Thank you so much!! You are always my inspiration! I do feel ridiculously positive and optimistic – I must have the good kind of brain damage =D Much love to you!
Knowledge is power and you are one of the most powerful women I have ever known. Keeping rockin’ it, Maggie. You are giving so much to so many people through your own journey, learnings, and stubborn refusal to roll over. You’ve got so much more to give–maybe that’s your best medicine. xOOx
Thank you Shirley! Your guidance through all this has meant so much.
Dear Maggie,
You are an incredible incredible woman!!
I know you know that but never hurts to be told and reminded of that over and over again.
You helped me and my partner speed up through our journey to keto, to metabolic process to believing and to keep going.
Thank you endlessly for that and I wish you and Bred from the bottom of my heart crazy universe support, loads of love, tons of your infectious optimism and energy and a healing journey further ahead to an even stronger you and happier you 2 together.
Lots of love & power from across the ocean!
Iva
Thank you so much, Iva!! That love and support mean everything. I’m looking out over Lake Union and Lake Washington to the Cascades and am just overwhelmed with love, joy and gratitude right now – and am sending it your way.
Dear Maggie,
Your fight with cancer is always so inspiring. I’m looking forward to your book to learn and be inspired. I wish you all the best and please do keep us updated in your blog or Instagram.
Much love,
Simpson
Wow! Thank you, Simpson! The book is really just a how to guide to implementing these incredible therapies for those already inspired. Your encouragement is what’s driving me!
Keep rockin’ it Maggie. We love you and Brad.
So much love to you and Angela!! I hope you saw the latest update – it’s not all that dire =D