I talk a lot about my GKI on this blog. I’ve been tracking it for about 10 months now and it’s taught me so much about the way my body metabolizes different foods and the way my metabolism reacts to certain events like stress, illness, and exercise. I credit most of my diet success to tracking as it’s helped me discover individual sensitivities like protein and processed food. Best/ worst of all, there’s no way to cheat a blood test!
I cover a lot in this article so feel free to skip to what’s relevant to you:
- What is the Glucose-Ketone Index?
- How do you calculate GKI?
- How do the results mean?
- Common factors that can impact your GKI
- Less known factors that can impact GKI
- How and how often should you test?
What is the Glucose-Ketone Index (GKI)?
The Glucose-Ketone Index was originally conceived by Dr. Thomas Seyfried and his team at Boston College to track overall metabolic health in cancer patients. It was quickly adopted as a benchmark for those with other metabolic conditions and anyone who wants to keep tabs on their metabolic health.
Your GKI is the ratio of your blood sugar to blood ketones at any given point in time.
Tracking blood sugar or blood ketones separately can also be useful but the ratio provides added insight and a quick benchmark for someone pursuing therapeutic ketosis, like me.
The results showed a clear relationship between the GKI and therapeutic efficacy using ketogenic diets and calorie restriction. The GKI is a simple tool that can help monitor the efficacy of metabolic therapy in preclinical animal models and in clinical trials for malignant brain cancer and possibly other cancers that express aerobic fermentation.
Meidenbauer, Joshua & Mukherjee, Purna. (2015). The glucose ketone index calculator: A simple tool to monitor therapeutic efficacy for metabolic management of brain cancer. Nutrition & metabolism. 12. 12. 10.1186/s12986-015-0009-2.
How to calculate your Glucose-Ketone Index (GKI)
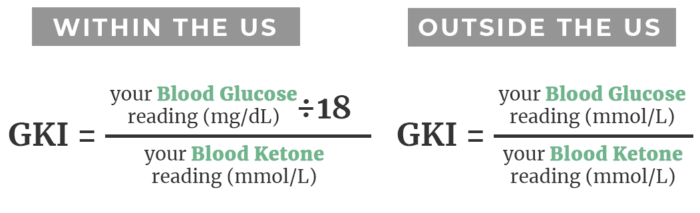
GKI is blood glucose (mmol/L) divided by blood ketones [BHB] (mmol/L). If you’re in the US, it is blood glucose (mg/dL) divided by 18 divided by blood ketones [BHB] (mmol/L).
First, you’ll need a blood glucose meter and a blood ketone meter. Blood glucose meters are pretty easy to find at any drug store and their test strips are usually inexpensive, as low as US$0.30 per strip. You may need to shop online for a ketone meter and those test strips usually run around US$2.00 each. I’ve been very happy with my keto mojo combined meter – just one pouch to carry around and the strips are around US$0.50 and US$1.00, respectively, on Amazon.
Getting a reading requires a little finger prick with the provided lancet and a 5-10 second wait for the results. Plug those numbers into the formula and voila, you know your GKI.
[ Get 15% off a Keto Mojo Meter Here. ]
After using it for about a year, however, I realized I could save a little money, keep track of fewer things, avoid the finger pricks, and get comparably accurate results with a Biosense breath meter.
[ Get $20.00 off a Biosense Breath Ketone Meter Here. ]
In the US, we generally measure blood sugar in mg/dL and blood ketones in mmol/L so we have to do a little conversion and divide the blood sugar reading by 18. In the UK or other countries where blood sugar is measured in mmol/L, it can be calculated as a simple ratio.
What do GKI results mean?
For therapeutic ketosis, the lower the GKI reading, the better. My goal is to stay under 1.0 for the majority of the day although some weeks I’ll relax and be satisfied with anything under 3.0. I’ve noticed that as I’ve become more fat adapted over time, it’s harder to stay in the sub-unity range without extended fasting. More on that below.
For folks pursuing nutritional ketosis for its general health benefits, anything under 9.0 is a good target.
What GKI numbers mean
| GKI | Reading | Application |
| 9 or above | Not in ketosis. | N/A. Just living a normal life. |
| 6-9 | Low level of ketosis. | For weight loss or health maintenance. |
| 3-6 | Moderate level of ketosis. | For managing Type 2 diabetes and obesity, insulin resistance, metabolic or endocrine disorders. |
| 1-3 | High therapeutic level of ketosis. | For those using keto therapeutically for the treatment of diseases such as cancer, epilepsy, Alzheimer’s, Parkinson’s, traumatic brain injury, etc. |
| less than 1 | The highest therapeutic level of ketosis | Very difficult to achieve without a doctor’s supervision. |


Most common factors that impact your Glucose-Ketone Index (GKI)
Amount of carbohydrate consumed
This one is obvious. Carbohydrates will raise your blood sugar. The first law of keto club is to reduce carbs. Your body won’t start breaking down fat to create ketones unless it’s running low on glucose. The general rule of thumb is to eat fewer than 20g net carbohydrates in order to enter this ketone-generating state known as ketosis. Net carbs are total carbs minus fiber and sugar alcohols as, supposedly, the latter don’t impact blood glucose.
How much you actually have to reduce carbs before you start creating ketones, however, depends on your individual body and the type of carbs you’re consuming, as below. GKI tracking can help you understand the right amount for you.
Quality of carbohydrate consumed
Not all carbs are the same when it comes to the metabolic impact. For many people, including myself, processed and refined carbohydrates have a much larger impact on GKI than those from whole vegetable sources. For example, I was able to maintain a GKI below 1.0 for months eating 45 or more grams of net carbs per day in the form of broccoli, kale, cabbage, and other vegetables (but, let’s be honest, mostly broccoli, kale and cabbage). On the other hand, if I cheat and eat a Quest bar with 4g net carbs, or some other low carb processed food – even if it’s the only thing I eat – my GKI will immediately spike and it usually takes me a day or so of fasting to get it back down.
I’ve read dozens of accounts from people whose experience mirrors my own in this regard. It probably isn’t an issue for most people pursuing nutritional ketosis but, if you find you’re not able to enter ketosis even at 20g or fewer net carbs, try cutting out the processed food and artificial sweeteners. Tracking your GKI during days eating only whole foods versus processed foods can tell you how your body reacts.
Artificial sweeteners are incredibly processed. You’ve never marveled at the beautiful fields of maltitol or spent childhood summers hunting for allulose in the woods. While some are better than others and each may affect you differently, be aware that they will likely have an effect on your GKI no matter what the label says. Also, for many people including myself, artificial sweeteners will increase appetite leading to cravings and negating the big appetite-suppressing benefit of keto. Of course, the only way to know for sure how artificial sweeteners impact you is to test.
Protein consumed
In addition to dietary sugar sources, the liver creates glucose from protein using a process called gluconeogenesis. This could happen during periods of true starvation when the body runs out of fat to use as fuel and starts to break down muscle for energy. More often, this is the process the liver undertakes when more protein is consumed than is needed for immediate energy needs and the body plans to store it for later energy needs in the form of fat.
In other words, too much protein can increase blood sugar leading to an increase in GKI. Most casual keto-ers don’t need to worry too much about their protein intake and some are more sensitive to protein than others. Nevertheless, virtually everyone trying to get into deep therapeutic ketosis will need to monitor their protein intake as closely as their carbs. GKI tracking can be an enormous help in finding the right individual amount of protein to consume.
Intense Exercise
Those of us committed to fueling our body with fat via ketosis rather than glucose will notice that it works. That is, after intense exercise, blood ketones are usually lower because they’ve been used for energy. Lower blood ketones leads to a lower higher GKI which is another way GKI can provide more data than testing ketones alone.
Even my mega chillax morning yoga practice usually lowers my blood ketones by .2-.5 mmol/L and increases my blood glucose by 5-10 ml/dL despite my not consuming any food.

Unexpected factors that can impact your Glucose-Ketone Index (GKI)
Stress and Conflict
This is surprisingly one of the biggest factors in my GKI monitoring now that I don’t have much variation in my diet. It’s part of the reason my mindfulness practices, yoga and mediation are so critical. A fight with Brad will send my blood glucose soaring 20 points or more and for weeks my morning GKI was elevated due to work stress.
It’s not just me. Diabetics have long been advised by medical authorities to monitor their stress levels to control blood sugar. Stress reducing activities like meditation, yoga, mindfulness practice, exercise, belly breathing and adequate sleep are all important parts of metabolic therapy and overall metabolic health.
Illness
Illness is a variation of stress, discussed above, and will affect your blood sugar in the same way. Additionally, if you’re dehydrated due to your illness the impact can be even more profound. Higher blood sugar means higher GKI reading even if you’re off food so drink plenty of water, rest, and don’t worry about your numbers until you feel well.
Sleep
I forget to include this one all too often because sleep has never been a problem for this girl. However, those of you who aren’t prioritizing 8 hours a night, aren’t observing good sleep hygiene or otherwise struggle to be fully rested will see the consequences in your GKI.
Gastroparesis
Though not common, gastroparesis, or delayed gastric emptying, can cause mysteriously high blood glucose readings until you figure out the cause. Delayed gastric emptying means the food you eat just sits in your stomach long, long after it should have moved along the digestive tract. It can be caused by inflammation, diabetes, neuropathy, some cancers and cancer treatments or other conditions that might damage the vagus nerve like MS or Parkinson’s. It’s a total bummer.
There are lots of fancy ways to diagnose it with trackers you ingest, etc. Simpler, just find yourself vomiting up the green salad you ate 2 days ago, still green, or carrying a food baby completely to term. I honest to God no exaggeration went out and bought a pregnancy test.
What’s worse, the treatment protocol for delayed gastric emptying recommends a diet low in fat and fiber with more frequent meals, completely the opposite of my intermittent fasting, plant-based ketogenic way of eating. I mean, all I eat is fat and fiber. And I prefer to eat it all in one sitting a day. Ultimately, I’ve managed to find tentative balance with smaller meals eaten more frequently between longer periods of fasting.
Adaptive Glucose Sparing
Adaptive glucose sparing is as much of a bummer for those pursuing therapeutic ketosis as gastroparesis. However, if you’ve noticed an unexplained rise in fasting blood glucose it could be the culprit. I intend to do a full post on this. In the meantime, the quick summary is that if you’ve been in deep ketosis for a long time, your muscles may come to prefer fat as the primary fuel and refuse available glucose in the bloodstream. Even if you eat a 0 carb diet your liver will still be making glucose via gluconeogenesis and, with no organs willing to use it as fuel, it sticks around in the bloodstream leading to higher blood sugar readings and thus higher GKI. This isn’t really a problem for most but for those of us using keto for cancer I imagine all that unused glucose goes straight to fueling metastasis. Not that dire, I’m sure, but still.

How often and when should you test your GKI?
This really depends on you and your goals. For me, there are three types of tracking that I find helpful: throughout select days, daily, and around individual events.
Track GKI Throughout the Day
I think that, for a few days at least, it’s helpful to test every 2-3 hours to develop an understanding of your natural patterns.
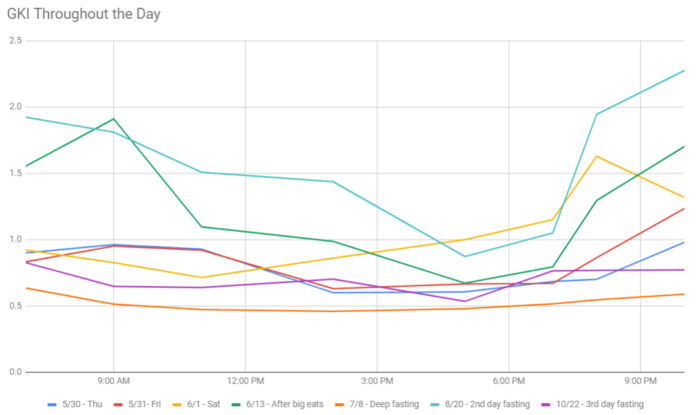
Each line in this graph represents my GKI over the course of a day from waking on the left to bedtime on the right. This type of tracking on “good” days and “bad,” fasting and feasting, helped me to identify normal and abnormal patterns over time. For example, the aqua line represents my second day water fasting when I’d expect to see something more like the orange or purple line. The fact that my GKI was so elevated despite not eating anything (and actually introducing metformin, a blood sugar reducing drug, to my regime) eventually led me to learn about gastroparesis and adaptive glucose sparing.
Daily GKI
Additionally, I like to keep a daily pulse on my GKI with a reading at the same time each day. For me, this is a few hours after waking when, as you can see from the chart above, my fasting GKI is at its highest. I also often include an evening measure prior to eating. Sometimes I’m strict about twice a day measures, especially when I travel and am introducing new foods. Other times I may go days without testing when I’m eating my usual diet and know the impacts.
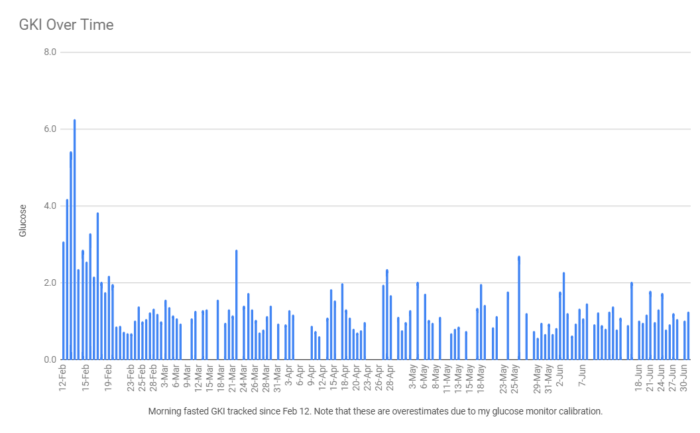
You can see in this chart of my GKI over time how much simply knowing my numbers helped me to recalibrate and improve them when I first started tracking.
This type of testing is especially helpful in identifying and understanding the impact of disturbed sleep or regular exercise on your metabolic health. Exercise may temporarily spike your GKI in the short-term but lower it over time.
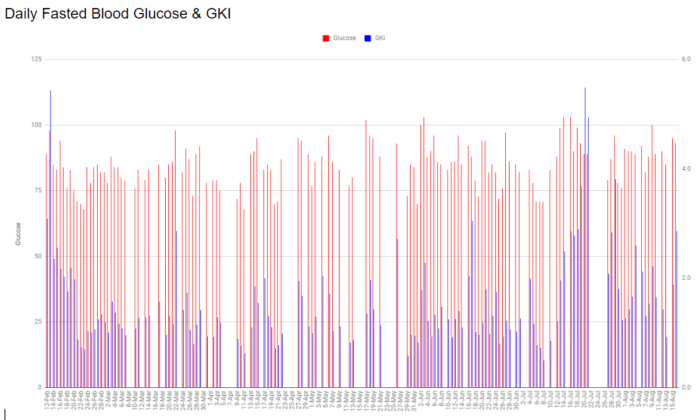
In the chart above you can see that daily tracking of my GKI (blue) revealed an issue much more clearly than just blood glucose alone (red). GKI clearly spiked and became elevated in August while the corresponding rise in blood glucose was less noticeable.
GKI Testing of Food and Activities
Finally, I find it enormously helpful to test the GKI impact of certain food and activities. To do this, I begin in a fasted state – at least 3 hours after eating although I usually start a minimum of 16 hours after eating.
Measure your GKI immediately before consuming the food or engaging in the activity in question, then at 30 minute intervals for the next 2-3 hours to see how your blood glucose and ketones respond. This is great for identifying sensitivities to certain foods like artificial sweeteners or processed treats. It can also uncover your body’s individual response to exercise, meditation, etc.

Final thoughts on GKI tracking for cancer and other therapeutic applications
Do it. If you don’t measure, you don’t know. I really don’t think its possible to effectively leverage ketosis for therapeutic purposes without tracking. There are so many personal factors that can affect your numbers its worth the small investment in your health to get a meter and test yourself regularly until you find your rhythm.
As the benefits of therapeutic ketosis are being scientifically demonstrated for more and more types of cancer, I don’t think it will be many more years before this is a standard part of cancer treatment testing.


36 comments
This is really interesting, thank you. I have a glucose meter I will buy a ketogenic one. Do you know if metastatic brain tumours are the same as lung to brain mets or glioblastoma tumors? I gave MBC with mets to spine, liver, eye and brain. I don’t know if I should be doing ketogenic?
Hi Collette! Not every cancer benefits from keto but breast cancer is one that seems VERY responsive. A study published in just September 2019 (this is all so new) compared two groups of 30 women each with late stage breast cancer requiring surgery. One group was treated with chemo only before the surgery, the other with chemo + keto. 30 months later, the keto+chemo group had 100% survival compared to 60% of chemo only. This was the first larger scale human trial but reaffirms animal studies and n=1 anecdotal evidence.
Wow! This is very interesting and good to know. Thank you.
Dear Maggie,
Thank you for this wonderful site. I have type 2 diabetes and was diagnosed with a 2 cm tumor invasive ductal carcinoma. I chose to go alternative with cancer and am alive and well after they said I would be dead by now (a year later). I test glucose & ketones for GKI and exercise twice daily.
I have a question that I wish could please be answered: Is therapeutic level GKI (less than 3) better than moderate level GKI (3-6) for type 2 diabetes? It is very easy for me to be in a therapeutic level, but I don’t have cancer anymore and am addressing type 2 diabetes.
Thank you in advance for the help!
seraphim
Seraphim, thank you so much for your kind words and for sharing your incredible story of healing. You are truly a miracle!
First, I’m not a doctor and it’s always wise to follow their advice. Personally, after crushing cancer, I usually advise a whole foods, plant-based diet incorporating more grains, legumes and fruits than are normally eaten on a therapeutic keto diet. It’s hard to advise on your particular case without knowing more details (let me know if you’d like to consult) but, if it’s easy to stay below 3.0 without incurring nutritional deficiencies, go for it!! You are an inspiration!
Have you noticed your GKI not being as favorable just before or during your period? I’m wrapping up a 36 hour fast and my numbers are in low level ketosis range, which is not normally the case for me. I don’t typically do any fasts longer than 18 hours on my period (or in the week before it) so I’m wondering if this could be the difference for me.
Holy smokes, Laura! Thank you so much! I cannot believe I didn’t address this here. Blood sugar and GKI are almost always higher immediately before and during your period, depending on the person, according to multiple diabetes research nonprofits. I happen to be expecting my period in the next day or two and am 36 hours fasted. I just checked my blood after reading this comment and indeed, my blood sugar is more than 10 points higher than usual at this point in the day and ketones are almost 1.0 mmol/L lower than I’d normally expect after a fast this long.
Honestly, I probably would have been pretty annoyed if I’d taken my GKI before getting your comment. Thank you so much for pointing this out! I’ll be updating the article to note how hormonal fluctuations can impact the GKI.
Congrats on your fast, too!
This is super helpful! Thank you! In addition to GKI I’m also curious with around what level your glucose is when you’re aiming for killing cancer? Because my GKI is good because my ketones are super high(4-6mmol/L) but my glucose is barely lower than when I wasn’t on keto and if lack of glucose is what starves tumors, then it seems like that might be a problem. Thanks!
Hi Bryce! That’s a great question and, if your ketones are in the 4-6 range, you almost certainly have a GKI around 1. A good reason to focus on the ratio rather than your glucose number is that you have less control over glucose – even if you ingested zero glucose, your liver will continue to create it using gluconeogenesis. Whatever your glucose, the ratio will provide insight into your metabolic health. For reference, my blood glucose most days is 84mg/dL – as high as 90s or low 100s after conflict or when sick, as low as 50s after days of fasting (but it can also be 80s during fasting). So really, I stay focused on the ratio as the true indicator of metabolic health and use the glucose numbers to help me troubleshoot any changes there.
Hope that is helpful!
Hi Maggie ! Thank You for putting up this website for I imagine it takes up a lot of time to do this. I just found out about the GKI. I started keto Nov 2020, stumbled upon intermittent fasting via youtube/keto and have been doing it for the last 7 months. I have lost a total of 50lbs. I started doing keto/IF with GKI for the last 2 weeks – I do not eat unless I am below a 3.
I am totally fascinated with this subject – you see during the last 2 weeks i have lost an average of 3.5lbs/week, but the previous 30 weeks , my average was 1.4lbs.
If this is what is doing for weight loss ,after 43lbs off, I am in awe of what it must be doing on a cellular level – I cannot get enough on this subject.
Just out of curiosity , what type of cancer were you diagnosed with ?
You have a great website , which I will be sharing with many .
Many Blessings
Alicia
Hi Alicia,
I was diagnosed with Stage 4 ROS1+ lung cancer metastasized to four tumors in my brain, two in my eye, one in my liver and dozens throughout the lymph nodes of my chest and abdomen. You can find more details including my scans at https://cancerv.me/2020/04/12/my-story-of-healing-from-terminal-stage-4-cancer/
You’re so right about the deeper healing benefits of ketosis – my husband follows my way of eating based on all we’ve learned. I’m currently working on a documentary exploring the powerful effects – more details on that at https://cancerevolution-movie.com/
Much love to you!
I have prostate cancer with Gleason score of 10. I’ve read that prostate and melanoma cancers are two cancers that feed on fat more than sugar. Is a keto diet advisable in either of these two cancers?
Hi Victor! I’m so sorry to hear about your diagnosis but inspired by the research that you’re doing! Sadly, I don’t think your question can be answered based on the tragic little research that’s been done to date. A survey of studies as of 2017 (read about it here: https://cancerv.me/2019/10/11/keto-for-cancer-benefits-and-downsides/) dug up 5 in vitro studies looking at prostrate cancer and found there was no effect in one, an anti-tumor affect in 3, and a pro-tumor effect in 1. Personally, I have a dear friend with a grade 5 prostate cancer who credits the metabolic protocol from Care Oncology with his current survival (https://cancerv.me/2020/08/15/the-care-oncology-clinic-protocol-for-metabolic-cancer-treatment/).
Of course, I can’t give medical advice under any circumstances. Speaking from personal experience, I’ve learned that all cancers can adapt their metabolism over time. That extra time has been everything for me.
Sending you the best!
Hi, does chemo affect your ketosis reading. I have chemo twice weekly for stage 4 cancer. My blood glucose is constantly around 5 but recently my ketosis number is only 0.6. I’m tracking all my food to your macros on cronometer, but I can’t get into ketosis again. Help!
Hi Katie! While there hasn’t been any real research on yet, my experience is that it absolutely does. The stress along is likely to raise blood glucose which will lower blood ketones and I’ve seen a pattern in some clients where ketones drop. There could be impacts from other medication, too – since starting steroids it’s been almost impossible for me to get my GKI below 1.0 – even after 3 days of water fasting my blood glucose is 140mg/dL where it used to be 84 on feed days. Sigh.
This isn’t medical advice, of course, but if I were in your position I’d look heavily into fasting – https://cancerv.me/2019/08/28/how-to-fast-and-why/
The benefits for potentiating chemo while minimizing side effects alone are amazing. It’s also the only essentially guaranteed way to drop GKI. Exogenous ketones like ketone esters may also help.
Sending good thoughts your way!
Maggie
I have searched for an answer to my question, without much success. I am able to achieve a low GKI through IF, but as soon as I put something in my mouth it shoots up dramatically. Example, just prior to eating today I tested and my GKI was 2.7 (Glucose 75 mg/dl – Ketones 1.5 mmol/L). Thirty minutes after eating, it was 10.6 (96 mg/dl – .5 mmol/L) and dropped to 8.3 (91 mg/dl – .6 mmol/L) over the next hour or so. I eat a very low-carb diet of <15g/day (~5-7%) and average around 78% fat intake of my daily consumption. Is it normal for my GKI to fluctuate to that degree or do I need to investigate further? I have only just started back to a keto/IF lifestyle (< month) so maybe I am just still working through my stores and fighting a little insulin resistance?? Thoughts?
Oof! Tracey! I’m so sorry to hear what you’re going through but know the frustrations all too well. My first question is what you’re eating to break fast. Your diet sounds awesome and the result of a ton of hard work and discipline – 78% fat is amazing. Can you test breaking fast with just a tbs of MCT oil in coffee? Then maybe with broth and wilted greens? Almost like an elimination diet to see what’s causing the spike. Any hidden sugar alcohols? Heavy protein?
I think your insulin resistance hypothesis is a really good one. There may be some food intolerances that contribute, too – things like seed oils, dairy, and factory meats have been known to have this affect. Also, are you taking any medication with your first meal? I need to update this article but some meds like steroids are almost hopeless to deal with (almost).
It really sounds like you’re on the right track, though. And no matter what, even with a spike up to the double digits for a while, all that time with GKI <3.0 is super healing! I'm so inspired!
Edit: Edit to add for folks who may find this in the future, it's not just sugar alcohols that can cause a problem but really anything sweet - even as innocuous as stevia leaf - can trigger an insulin spike. Really a pain, I know!
Maggie, thank you so much for the quick response!
I do add MCT oil to my last cup of coffee, which is usually about 45 minutes before I break fast around 12-12:30. My first meal of the day usually consists of a salad with lots of goodies added in and about 3oz. of protein (salmon, shrimp, tuna, steak sometimes) I add chia seeds, nuts and usually top with olive oil.
I used to eat on the heavier side of protein, but now no more than 3oz per meal, maybe twice daily. I do my best to only consume grass-fed/grass-finished, free ranch, ethically raised (you get it). I watch labels pretty closely and avoid added sugars and do my best to avoid any naturally occurring sugars, if possible. I avoid grains, legumes and the sugars as mentioned. Only oils I use are EVOO, avocado and coconut oils. I occasionally use ghee or grass-fed butter. I cook about 95% of our meals at home, as clean as I am able.
I do not take any medications with my first meal.
I am at a loss on how to have a much more positive impact on the numbers and keep them steady. I will definitely need to pursue intolerances, as that may very well be the culprit. I will try your suggestions for sure.
Today’s numbers were a little better, but much of the same story. Woke (tested after 2 hours – dawn effect) and was 8.8 GKI. Tested again right before lunch hour and was 2.2 GKI. That’s still good, but confusing.
Thank you again! You and your story are so very inspiring and I am thankful I came across your blog. Such a great resource!
First, just hearing about your diet brings a smile to my heart! And like you say, your numbers are great so it’s really just curiosity now. My advice would be to try your noon meal without the protein. Some folks (like me) are super sensitive to protein – it spikes me more than whole veg carbs. You need it, obviously, and you’re eating the right healing sources, so this would just be to confirm that it’s the cause of the spike and set your mind at ease.
Please let me know! I’m really blown away but what you’re doing here!
Hello Maggie,
Thank you so much for your fabulous site. I just started reading. So forgive me, if the answers to my questions are somewhere to be found on your website.
I recently had surgery for stage 2 breast cancer. The margins are good, the lymph nodes are clear. I have decided to forgo the suggested allopathic follow up treatments since I am really healthy otherwise.
So now the question is: where do I take it from here? Low carb intake is a no-brainer I think. I have started with intermittent fasting because the concept of autophagy makes so much sense to me. I have also started with more of a keto diet without measuring anything at this point. (Will look at the meters).
There are two issues though:
I have no weight to loose and find it a bit hard to keep the pounds on. How does one get from glucose metabolism to a more flexible metabolism without loosing weight?
The second questions stems from something I just read here. You are suggesting a plant based diet for cancer after- care. I used to be a plant based eater and feel much better on my present diet.
Thank you kindly for your response!
Hello Maggie,
Thank you for sharing your amazing info, research and experience.
I just had breast surgery for stage 2 cancer, good margins and clear lymph nodes. I made the decision to forgo any allopathic follow up treatments, thus my interest in the right diet (which started as soon as I got the diagnosis).
I have two questions:
– I have started to experiment with intermittent fasting because the concept of autophagy makes so much sense. I’d love to do even longer fasts for the health benefits. Yet I am a lightweight with no pounds to lose. Can the body learn to build metabolic flexibility without losing weight? My diet is veggies veggies veggies, healthy fats, some good quality animal protein, nuts, berries and once in a while some oatmeal, cocoa nibs…
– I just read on this page that you are suggesting a plant based keto diet for cancer after care. Can you explain why? I used to eat plant based and feel much better on my present diet.
Thank you kindly!
Hi Kerstin!
You story and the research you’ve done are inspiring. I’m so excited for your continued healing!
– I’ve worked with many clients to leverage metabolic therapies who aren’t in a position to lose weight. It’s more challenging but absolutely possible to eat a ketogenic diet and incorporate fasting without losing weight (after the initial water loss and assuming the subject isn’t overweight). It may require eating even when you don’t feel hungry and incorporating more of those healing, energy-dense foods: nuts, avocado, coconut oil, coconut milk, chia seeds, flax seeds, cacao. Alternating deep keto/ fasting days with higher glucose days can also help. I’m actually working on a video about strategies that have been successful for my clients that I hope will be done end of this year. The weight gain secret for me and my husband this past year has been too many nuts =D
– Each individual has incredibly different needs as far as animal protein. For me *personally*, a plant-based diet with only 5-10% of calories from animal products (the definition of plant-based). For me, I find organic, pasture-raised eggs and wild-caught fatty fish is most healing and helps me prioritize the right plant and animal micronutrients while staying within my personal protein macro limit to manage my GKI. I’ve worked with clients with much higher protein needs which we determine through tracking macros, GKI levels, other bloodwork and how they feel. My only universal recommendation is to avoid factory meat as much as possible in favor of organic grass-fed , grass-finished ruminants or, if weight-gain is a goal, meat with more linoleic acid like pasture-raised poultry. There have been several studies correlating factory meat with cancer. While beyond the scope of this comment, it’s individual and complicated and involves many factors. I’ve only shared my personal experience here but look forward to outlining more complete learnings based on anonymized experience by the end of the year. For now, it sounds like you’re listening to your body and doing what’s right for you.
Much love!
I think Dr Seyfried is at Boston College, not Boston University. Two completely different schools.
Thank you so much for catching! I’ve corrected it thanks to you.
I was so lucky to visit his lab at Boston College earlier this year for the documentary. I won’t make the mistake again.
Excellent article — really appreciate the summary. Under Intense Exercise, the text states, “Lower blood ketones leads to a lower overall GKI…” If I understand the mathematics correctly, shouldn’t it be “…higher overall GKI…”? In any event, thanks for this!
Oh geez! How did I miss that? Thank you so so much! Correcting it now.
Maggie –
Wonderful site! Thank you so much for all you share. Quick question on GKI… as far as you know, is there any danger in maintaining a GKI below 3.0? It’s recommended for severe conditions only, and not just for weight loss and general health, but is it potentially harmful to those not undergoing treatment?
Hi Brian! Great question! As I’ve seen, over the long term, constant low GKI might lead to things like physiological insulin resistance (adaptive glucose sparing discussed above) and hormonal issues in pre-menopausal women. I don’t know that either condition is really dangerous but it’s part of the reason I prefer a goal of “metabolic flexibility.” I’ve also had multiple clients who find <1.0 GKI very easy but that experienced a high anion gap leading to low BUN ratio in their bloods. I advice these clients to bring their GKI higher. Also, tumors can adapt to use ketones to fuel their growth instead of glucose but I feel that the other benefits of ketones outweigh this concern. Personally, staying <3.0 through my year of healing (and <1.0 half the week), was important to me. Now that I've been cancer free for three years, I alternate periods of deep ketosis (<2.0 GKI) with extended water fasting and periods where I include fruits, sweet potatoes, carrots, and other starchy veg. Even legumes and pseudo-grains (buckwheat and quinoa) a few times.
Ultimately, there's far too little research. Listen to your own body, watch your labs, and consult with your medical team and all that =D Good luck!
Maggie, I love your website; I don’t think there is one comment from which I didn’t benefit immensely, and I thank everyone for his/her generosity in sharing his/her experiences and thoughts. I have one idea based on reading recent articles concerning the II (insulin index) of foods, proteinaceous ones in particular. While it’s not exactly news, it is not well publicized and, it seems to me, is largely ignored: most animal proteins SPIKE insulin (while having little effect upon sugar levels). How weird is that? Not much seems to have been written or researched about this, so I am only speculating that a high protein diet might have a negative impact upon ketosis. Insulin depressing ketogenesis and all. I became interested in this because I have insulin resistance and weight gain issues, and I have been experimenting with ways to to decease insulin production. I don’t seem to be able to manage fasting very well at all, but with care and precaution am managing Mosley’s 5-2 IF program, eating essentially a 3-10-87 diet on a 16-8 daily schedule. My fasting BS has dropped into the 90’s, my A1c is 5.3, and on 500-Cal fasting days, my ketones are 3 and higher. My GKI after 24 hrs of modified fasting has been 1-2; my weight has been stable at a higher caloric intake. I had prediabetic metrics for a couple of years before now and have tended toward carb intolerance; I have followed a very low carbohydrate (if not always ketogenic) diet for over 2 years; I consider my current diet mainly therapeutic, unhealthy as a long term strategy; it’s extreme and I offer this information only as data input, not as a solution to any kind of metabolic disorder. Best wishes to you all, laurie
Hi Laureen! Thank you so much for the kind words and encouragement! And your personal story is amazing! Wow, what an accomplishment!
YES! Your info on the effect of animal proteins on insulin (regardless of their effect on glucose) is so helpful and something I should write a full post on. When I first wrote this post, I was working from my own little n=1 experiments. Since starting a practice to work with others, I’ve learned that not everyone sees the same glucose spike from protein that I do. Even more important that we understand what you’re pointing out – that insulin can spike regardless.
3/10/87 is no joke (and no fun) but wow, your disciple is paying off! You are an inspiration! Thank you for contributing here!
HI Maggie, thank you for sharig this valuable and insightful information. I am doing somewhat the same thing, now I am have put enough knowledge together for a better understanding of GKI, and a goal of going into a deeper state. I do track throughout the day too. Most of the time I maintain in the 2. something range, and have been under 1.0 during a five day water fast. Your explaination for Adaptive Glucose Sparing was insightful. Best Wishes to you!
Wow, Rick! Thank you for the kind, encouraging words! Keeping a GKI <2 and <1 on extended water fasts is an amazing feat - I know how much dedication it takes and I'm so impressed. Wishing you the best on your journey!
Hi Maggie ,
Hope you’re very well !!! You’re an inspiration for all of us!
Just been told have lung cancer with genetic mutation so I’m lucky enough to be in a clinical trial. I’m trying to keep ketones low by following your tips and diet. Really cannot. What am I doing wrong? Thanks
Hi Ilaria! Alas, without WAY more details I can’t say but I strongly recommend you consult with a nutritionist versed in therapeutic keto. See https://cancerv.me/faq/ for some recommendations. Every body is different and no diet is optimal for everyone. It could be anything from genetic SNPs requiring more animal protein/ fewer carbs, feeding window, calories, etc. Ketosis isn’t possible for people of Inuit heritage. Steroids can make it virtually impossible.
One thing to get everyone else into deep ketosis is water fasting. However, there are contraindications for this as well. I can’t recommend strongly enough consulting with your metabolically-informed practitioner. Sending all my love!
Thank you for sharing such valuable and detailed information, I truly appreciate your time, energy and effort! Can you please tell me if the graphs above tracking your ketones and glucose readings are from Cronometer? Are they included in the paid version of the app?
Hi Rochelle!
I make those graphs manually in excel. Would be awesome if cronometer did something similar!