This one is good.
My lorlatinib instructions are to take 4 25mg tablets once per day. I thought that was weird since I know they make a 100mg tablet. What’s the medical value of taking 4 pills at a time rather than just one?
A 30-day supply of 25mg tablets (120) costs $21,630.41.
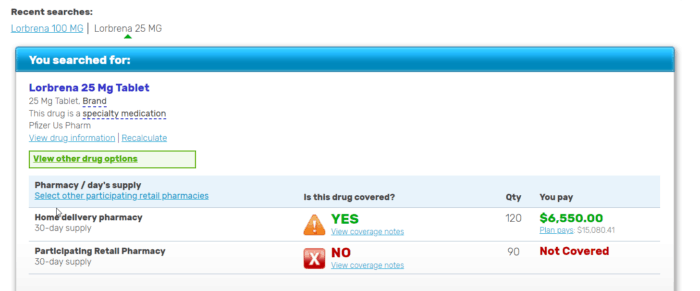
A 30-day supply of 100mg tablets (30) costs $16,222.79.
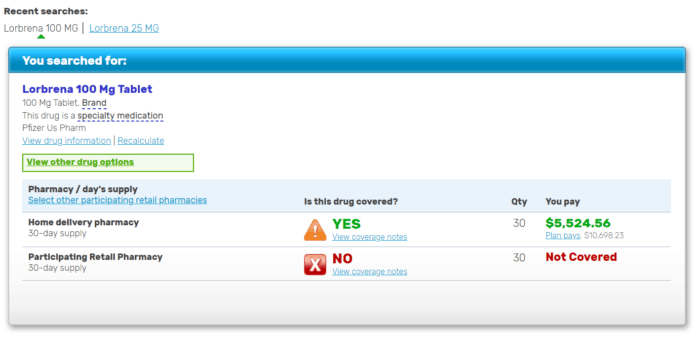
These are all US dollars.
I braved the pharmacy phone tree and three disconnects to ask them to make the change to 100mg tablets. They told me the tablet size had been specified in my prescription. I will bet a month’s worth of lorlatinib those poor doctors at the Mayo Clinic have no idea about costs and are just doing what’s recommended as “best practice” by the drug manufacturer. I sent them an email and hope they’re willing to deal with the god-awful phone tree to make the change.
The pharmacy “customer advocate” didn’t understand why I even cared about the price since my current copay is $0. My current copay is $0 because, after many, many hours of research and phone calls I’m fortunate to have Pfizer Copay Assistance, but it only covers up to $25,000 a year. The faster I blow through that $25k the faster I’m paying those beefy copays myself.
The customer advocate still didn’t quite appreciate my concerns. It might be relevant to note that this pharmacy, Accredo, is wholly owned by Express-Scripts, the pharmacy benefit manager mandated by my insurance. They’re the only pharmacy I’ve found that will accept Pfizer Copay Assistance, though, so, full circle.



4 comments
Wow! Talk about injustice! So frustrating! It’s also frustrating that their rep was either playing dumb or actually didn’t get it. So sorry Maggie! Love you!
Thank you so much, dude! At this point this kind of stuff doesn’t even bother me anymore. I’m a tourist in this cancer world and these are the sights. Much love to you and the girls!
Hi Maggie,
Firstly, I wanted to thank you for this website. It has been so incredibly helpful. I hope you’re doing well!
This post is a few years old now so I am not sure you will see this comment, but I thought I’d ask just in case. My Mom is currently undergoing chemotherapy (1x/week, intravenous cisplatin) and radiation (daily). She just started yesterday and has been feeling really sick. She has been fasting once/week (36 hours) and eating a ketogenic diet since the end of July. What has been challenging is figuring out how to approach the anti-nausea medications she has been prescribed while continuing to fast prior to treatment, when she has been directed to take the meds an hour before chemotherapy, for example. I wanted to ask whether you took any antiemetic meds and if so, whether that meant you weren’t fasting on those days so as not take them on an empty stomach. The use of these medications themselves is hard to wrap your head around in the face of research showing their immunosuppressive effects and potential to counteract the effects of chemotherapy/radiation. It feels like choosing the lesser of two evils. If you could share any insight on this, that would be greatly appreciated. All the best!
Hi Maria, I’m so sorry for what you and your mother are going through and am sending you love.
My advice is not the best here. I’m not a doctor and you should consult your medical team and all that. My personal experience is that when I researched the antiemetic meds I was prescribed, they didn’t seem in my best interested and stopped taking them. To this day I do not take food with my morning medications that I’m instructed to eat with. I found my own clinical research that Boswellia had a steroid-sparing effect and got off the dexamethasone. I do keto against my doctor’s orders; I take off label drugs they refuse to prescribe; I fast and do HBOT against their instructions (although they finally got on board with HBOT). In short, my prognosis was so bleak (months) that I felt empowered to do what I thought was best for me based on my research and not what the doctors told me to do. In my small, personal experience, I know that was right but is not something I can preach to others – except for your mother to do what she feels is right for her.
Sending love! Maggie